Dr Charlotte Squires was diagnosed with advanced Hodgkin lymphoma in November 2018 when she was 30. In this guest blog post, she writes about how her diagnosis and treatment has changed the way that she approaches her career as a doctor.
Lymphoma is known for being tricky to diagnose: it can present in strange ways, or with signs that may not seem that concerning to people without medical knowledge.
As a doctor, it was surprisingly easy to work out what was going on. My partner and I were living and working in New Zealand on a year out between stages of my UK medical training when I realised that I was losing weight. Initially I was pleased, as many of us would be, and I put it down to healthier eating. But then the weight kept coming off, the night sweats began, and it started sounding less like a reason to buy new skinny jeans, and more like a cancer diagnosis waiting to happen. I wrote a list of what I thought could be wrong – each illness more worrying than the next – and took it, terrified, to my own GP. He thought I was just anxious but he took some blood tests anyway, expecting to be reassured. The next day I was on call at the hospital, seeing acutely unwell patients in the emergency department, when my GP phoned. My results were more abnormal than those of the patients that I had spent the morning admitting, and they were highly suggestive of cancer. Over the next week I had a CT, then a biopsy, and then confirmation of advanced lymphoma – the illness that had been at the top of my worrying list. packed up our things in three days and flew home. I found myself tipped from the end of the hospital bed, headfirst into it.

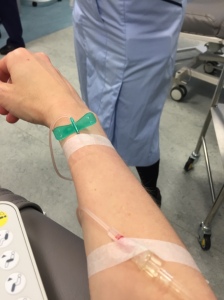
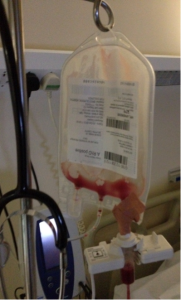
Charlotte during treatment for Hodgkin lymphoma
Becoming a doctor involves a lot of learning. Medical professionals spend long years memorising anatomical diagrams, the routes of nerves and blood vessels, the causes of different symptoms, and what different organs look like under a microscope. We spend hours speaking to patients, trying to understand what it means to have an illness and to undergo treatment. We learn about drug doses, side effects, and the likelihood of successful treatment. We learn how to break bad news, and how to explain complex diseases.
And yet, there was so much I didn’t know.
I didn’t know what it means to have a mouth so sore that you can’t bear to drink. I didn’t know how it feels to lose all of your hair on your birthday, or how hard it is to know that it will take several years to grow back fully. I didn’t know the paralysing misery of severe nausea, or the gripping pain from bone marrow-boosting injections, or what it’s like to nearly faint in the middle of the Aldi Christmas aisle due to severe anaemia. I didn’t know how it feels to face down your mortality, or to lose friends, young and beautiful, to terrible illnesses similar to your own. I didn’t know what it was like to feel afraid, and so vulnerable that it’s as though your skin has been flayed from your bones. I didn’t know just how often the health service gets it wrong, or sends things astray, or just forgets, and how sometimes it doesn’t really seem to care. I didn’t know what it means to feel unable to trust your own body. I didn’t know how much bravery it takes, every day, to live with and through a cancer diagnosis. There is much I’ve had to learn.
I’ve learned what it means to wait, like Schrodinger’s patient, both relapsed and in remission at the same time, until the scan result arrives. I’ve learned how to sit anxiously, in quiet waiting rooms, afraid of what might happen on the other side of a closed door and wondering whether I’ll be able to find the words to tell my family if it’s yet more bad news. I’ve learned to try to sit with this, to own it, and to keep living whilst I wait.
I’ve learned what it means to be unable to plan ahead, or to have multiple caveats around treatment timelines, scan results, and the major impact of fatigue. I’ve learned what it means to cancel an anniversary dinner at the last minute after vomiting spectacularly in a restaurant car park, and how it feels to be the awkward one with special requirements, who needs others to be flexible, and who can no longer work those long hours without a second thought.

Our blog author Charlotte
Now, eight months later, after four cycles of chemotherapy and more tablets and injections than I care to remember, I am back at work, on the easiest end of the stethoscope. My hair is slowly growing back, and I am beginning to feel more normal. But it is a slow process, full of peaks and troughs and unexpected detours. As a patient, I was often frustrated. As a doctor, I try to look for those frustrations and acknowledge them, even if I can’t always fix them. One of the biggest things I often think about is how as a doctor, I see my patients for 20 minutes in clinic and often have little knowledge of their lives beyond the hospital walls – and of what it means to have your life suddenly turned upside down. These days I try to ask, to listen to the stories, and to say, honestly, that managing illness takes more effort than treating it. As doctors, we’ve learned a lot to get to where we are, but there is still so much that we don’t know.